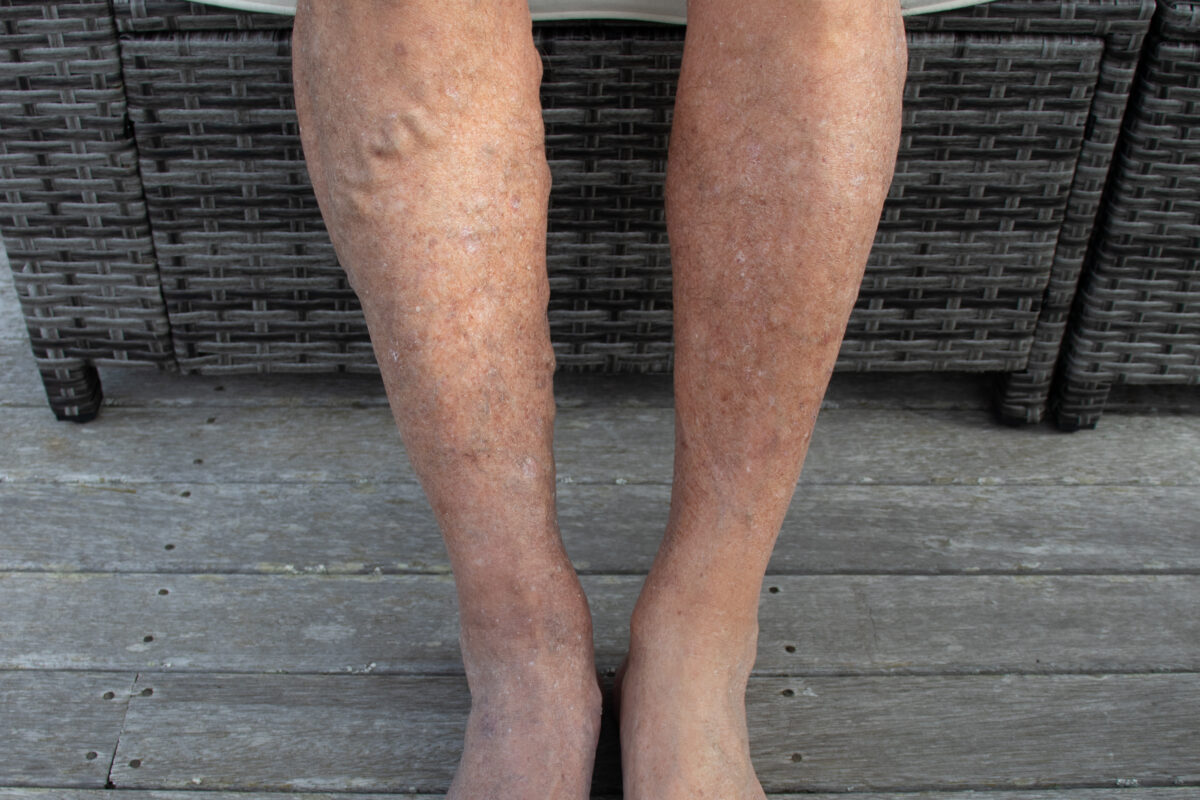
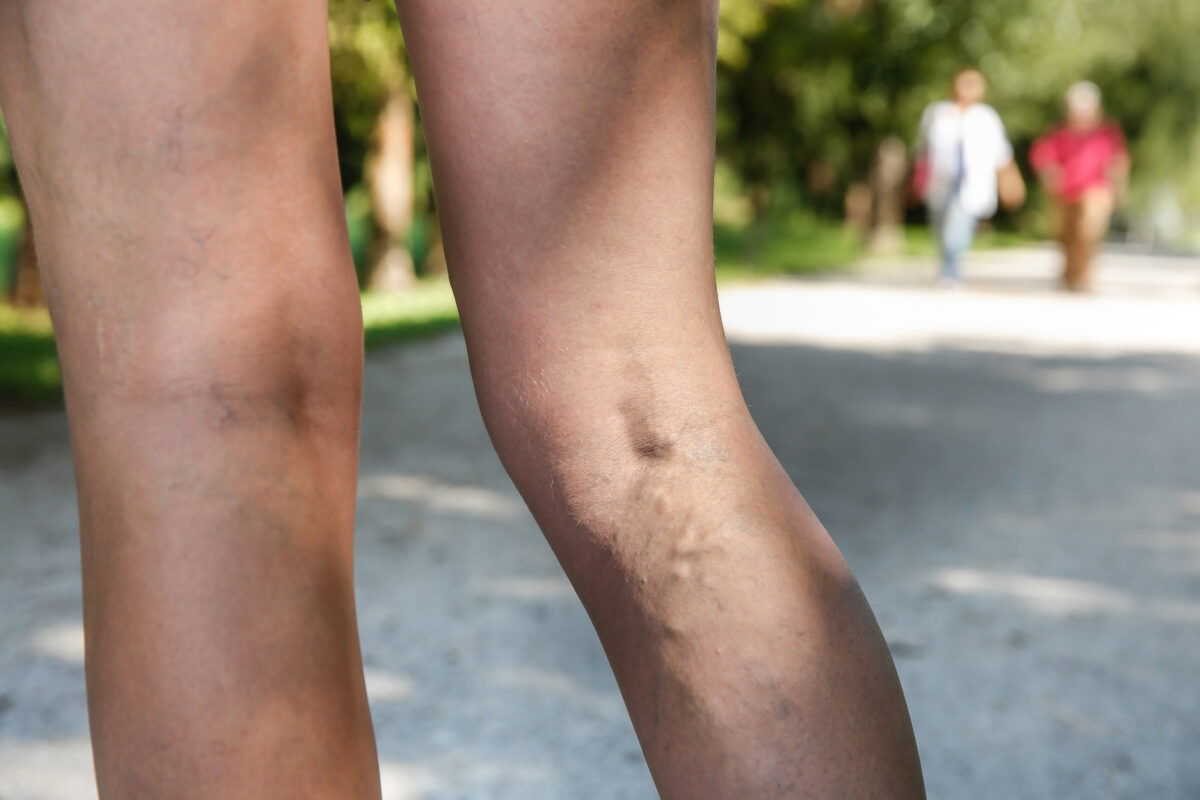
Your body’s lower-half poses a genuine challenge to daily blood flow, making most people vulnerable to leg circulation issues.
Gravity works against the return trip, constantly pulling blood downward while your body counters with tiny valves and carefully managed pressure shifts. Even minor disruptions to this balance can have real consequences.
Excess sodium has quietly become one of the most common disruptors. It infiltrates far more meals than most people recognize, often hiding in foods that don’t taste particularly salty. Your nerves and muscles depend on salt, but when consumed in excess, sodium alters how blood vessels behave, gradually increasing the strain on the veins running through your legs.
The typical Western diet delivers far more sodium than the body can efficiently process, and that chronic overload doesn’t announce itself loudly. It builds slowly, subtly, and often goes unnoticed until the damage is already underway.
Understanding these patterns is where good health begins. What you eat and how often you move accumulates over time and ultimately shapes how your body functions from the ground up.
Edema, the RAAS Impact, and Leg Circulation Issues
Excess sodium disrupts the way fluids move through your blood vessels, and the legs tend to bear the brunt of it.
In general, salt behaves like a magnet for water. When sodium in your blood rises after a salty meal, your body responds by pulling water out of cells and into the bloodstream. That added volume increases pressure against vessel walls that weren’t built to handle the surge.
Because gravity works against circulation in the legs, that pressure accumulates there first. Fluid gets pushed out of the vessels and into the surrounding soft tissue, which is why ankles swell — particularly after high-sodium meals.
Here’s a simple test: press your finger into the swollen area. If it leaves an indentation, your vessels are struggling to retain fluid where it belongs. That pitting is a visible sign that your body is losing the battle with excess salt.
Sodium’s impact runs deeper than basic osmosis, though. It activates the Renin-Angiotensin-Aldosterone System (commonly called RAAS), which governs long-term blood pressure and fluid regulation.
When specialized kidney cells called juxtaglomerular cells detect elevated sodium or rising blood pressure, they release an enzyme called renin. Renin breaks down angiotensinogen into Angiotensin I, which an enzyme called ACE then converts into Angiotensin II.
Angiotensin II binds directly to muscle cells lining the leg arteries, causing them to constrict. Narrower arteries force the heart to work harder, and blood flow to the legs can drop noticeably as a result. Simultaneously, Angiotensin II signals the adrenal glands to release aldosterone, which instructs the kidneys to retain sodium and excrete potassium instead.
This creates a self-reinforcing loop. The body holds onto more water, vessels stay chronically tense, and veins swell from the extra volume while arteries struggle to deliver adequate blood flow.
For people who are salt-sensitive, this cascade is what produces those familiar feelings of heaviness and discomfort in the legs.
Salt and the Endothelial Glycocalyx
Research has identified a thin protective layer lining the inside of blood vessels, called the Endothelial Glycocalyx, which plays a role in preventing leg circulation issues.
You can think of it as a soft, protein-rich coating that covers every artery and vein, functioning simultaneously as a sensor, a buffer, and a selective barrier between flowing blood and the vessel wall. Despite being barely thicker than a strand of hair, it plays an outsized role in vascular health.
Excess sodium degrades this layer. High sodium concentrations cause the glycocalyx to break down, shedding fragments into the bloodstream and leaving the underlying vessel wall exposed.
That exposure has real consequences. Vessels stripped of this coating lose much of their ability to produce nitric oxide, a chemical that signals smooth muscle in the leg vessels to relax. Without adequate nitric oxide, those vessels remain in a persistently constricted state, often without any obvious symptoms in the early stages.
Damaged vessel walls also become stickier, allowing white blood cells to adhere and triggering low-grade, chronic inflammation. Over time, the vessels stiffen and lose the flexibility that healthy circulation depends on.
“Endothelial glycocalyx loss happens through the aging process and repairing the endothelial glycocalyx may alleviate the symptoms of age-related diseases,” states Aging and Disease. “Given the important role of the glycocalyx and its regenerative properties, it is posited that the endothelial glycocalyx may be a potential therapeutic target for aging and age-related diseases and repairing endothelial glycocalyx could play a role in the promotion of healthy aging and longevity.”
Recovery isn’t immediate, either. After a high-sodium meal, compromised leg circulation doesn’t simply bounce back once the meal is over. Rebuilding the glycocalyx takes time — potentially several days of reduced sodium intake before the protective layer meaningfully restores itself.
The ‘Salty Six’ and the Modern Grocery Trap
The American Heart Association has flagged what it calls the “Salty Six,” a group of foods that carry enough sodium to impair blood flow and contribute to leg circulation issues. Regular consumption of these foods can drive inflammation in blood vessels, compounding your vascular stress:
- Breads and rolls. A single slice can contain 230 milligrams of sodium. Many people consume multiple servings daily.
- Pizza. The combination of processed dough, high-sodium cheese, and nitrate-heavy meats creates a massive osmotic load.
- Sandwiches and wraps. Hidden sodium lurks in the sauces, bread, and deli meats.
- Cold cuts and cured meats. Producers often use sodium nitrates to preserve these, which specifically damage the endothelial lining.
- Soup. A single can of “healthy” vegetable soup can contain over 1,000 milligrams of sodium.
- Burritos and tacos. Seasoning packets often consist of nearly 50 percent sodium by weight.
A walk through any grocery store makes the problem obvious. Sodium isn’t confined to obviously salty snacks. It’s embedded in bread, canned soups, deli meats, and even pre-seasoned raw poultry.
Most packaged foods contain more sodium than the label implies at a glance, which makes unintentional overconsumption remarkably easy.
“Despite what many people think, most dietary sodium (over 70%) comes from eating packaged and prepared foods — not from table salt added to food when cooking or eating,” according to the U.S. Food and Drug Administration (FDA). “The food supply contains too much sodium and Americans who want to consume less sodium can have a difficult time doing so.”
For anyone already experiencing numb legs or chronically swollen feet, this goes beyond general wellness advice. Reducing sodium intake becomes a practical and targeted intervention, not an optional lifestyle upgrade.
Left unaddressed, those symptoms can worsen progressively, and the underlying vascular damage continues accumulating in the background.
Choosing Blood Flow Over Swelling and Leg Circulation Issues
Improving your leg circulation issues starts with something as straightforward as reconsidering what you snack on.
Reducing sodium intake is a practical first step, and swapping high-salt options for foods rich in potassium or fiber makes that shift easier. Eat fresh fruit instead of chips, and unsalted nuts instead of their processed counterparts.
These aren’t dramatic sacrifices, but they consistently move the needle.
| Food Category | High-Sodium Culprit | Circulation Alternative | Vascular Benefit |
| Lunch | Deli Turkey Breast | Fresh Roasted Chicken | Reduced nitrate-induced inflammation |
| Grains | Store-bought White Bread | Flourless Sprouted Bread | Lower glycemic index and reduced sodium |
| Snacks | Salted Pretzels | Raw Walnuts/Almonds | Omega-3s support endothelial health |
| Flavoring | Soy Sauce | Lemon & Fresh Ginger | Ginger acts as a natural vasodilator |
| Vegetables | Canned Peas | Fresh/Frozen Spinach | High Potassium to flush sodium |
| Breakfast | Instant Oatmeal Packet | Steel Cut Oats w/ Berries | High fiber and natural antioxidants |
As sodium levels drop, the body responds in measurable ways. Blood flow improves gradually, legs feel noticeably lighter, and swelling becomes less frequent and less severe.
Healthier, more flexible vessels translate directly into reduced fatigue and discomfort.
A Vascular Crisis in Numbers
The World Health Organization set a global target to reduce salt consumption by 2025, largely as a strategy against cardiovascular disease. Currently, most people consume more than 10 grams of salt daily — double the 5-gram ceiling that health authorities recommend.
In the United States, the numbers are particularly stark: nearly 9 in 10 people regularly exceed safe sodium limits.
That excess takes a quiet but measurable toll on leg circulation. Approximately 8.5 million Americans live with Peripheral Artery Disease (PAD), a condition that high sodium directly worsens by stiffening arterial walls and restricting blood flow. Most people don’t recognize the problem until the damage is already well established.
Consider anyone who spends most of their days on their feet. By evening, their socks leave deep impressions on their ankles, and a dull ache with occasional numbness settles into the lower legs. Many attribute it to their long hours, which is a reasonable assumption but an incomplete one.
Their meals don’t look problematic on the surface: a low-fat muffin in the morning, a turkey sandwich at lunchtime, and frozen pasta for dinner. Unremarkable on the surface, yet by the end of the day they’ve consumed roughly 4,500 milligrams of sodium.
That load prompts their bodies to retain water, which accumulates in the lower legs, compresses the small surrounding blood vessels, and measurably slows circulation.
What these people actually need is a sustained reduction in sodium. Only when that intake drops can they begin retaining fluid and restoring normal pressure in the vessels throughout their legs.
The DASH Approach and Potassium Counter-Balance
The DASH diet has earned its reputation for addressing leg circulation issues largely because it tackles two variables simultaneously: keeping sodium low while ensuring adequate potassium intake.
These two minerals work in direct opposition inside the body. Sodium promotes fluid retention, and potassium signals the kidneys to excrete sodium and helps blood vessels maintain a relaxed, open state.
A useful target is a 2:1 potassium-to-sodium ratio — at minimum, two milligrams of potassium for every milligram of sodium consumed. Foods like sweet potatoes, spinach, avocados, and white beans deliver potassium in meaningful amounts.
Consistently hitting that ratio helps push accumulated fluid out of the legs and supports more efficient blood flow through the vessels.
“On the DASH diet, you can eat foods from all food groups,” states MedlinePlus. “But you will include more of the foods that are naturally low in salt, cholesterol, and saturated fats. You will also include foods that are high in potassium, calcium, magnesium, and fiber.”
Here’s a list of the food groups and how many servings of each you should have per day, according to the article. For a diet that has 2000 calories per day, you should eat:
- Vegetables (4 to 5 servings a day).
- Fruits (4 to 5 servings a day).
- Low-fat or fat-free dairy products, such as milk or yogurt (2 to 3 servings a day).
- Grains (6 to 8 servings a day, and 3 should be whole grains).
- Fish, lean meats, and poultry (2 servings or less a day).
- Beans, seeds, and nuts (4 to 5 servings a week).
- Fats and oils (2 to 3 servings a day).
- Sweets or added sugars, such as jelly, hard candy, maple syrup, sorbet, and sugar (fewer than 5 servings a week).
Processed foods are the primary obstacle here. They tend to carry heavy sodium loads that quietly tip the balance in the wrong direction, contributing to swelling, vessel tension, and reduced circulation over time.
Shifting toward whole, minimally processed foods recalibrates your balance and your legs. Remember: your body’s legs bear the full weight of circulatory strain every day. They’re usually where the improvement shows up first.
Frequently Asked Questions: Leg Circulation Issues
- How long does it take for leg swelling to go down after reducing salt? You may notice a reduction in acute fluid retention within 24-48 hours of lowering sodium and increasing water intake. However, if chronic damage affects the vein valves, the body may require several weeks of a consistent DASH-style diet to see permanent improvement.
- Does drinking more water help if I have already eaten too much salt? Yes. Hydration is key. When the body experiences dehydration, it holds onto sodium more aggressively. By drinking water, you signal to the kidneys to excrete the stored sodium through urine.
- Can I just take a water pill instead of changing my diet? You should only take diuretics (water pills) under medical supervision. While they remove fluid, they do not repair the endothelial glycocalyx damage. A dietary approach treats the root cause — your vascular health — rather than just the symptom of fluid pooling.
- Are all salts the same? Is sea salt better for circulation? From a sodium perspective, yes. Himalayan pink salt, sea salt, and table salt all contain roughly 40 percent sodium. Their impact on fluid retention and the RAAS system remains identical.
Wellness and Pain
Fix your leg circulation issues by visiting Wellness and Pain. We offer conservative treatments, routine visits, and minimally invasive quick-recovery procedures. We can keep you free of problems by providing lifestyle education and home care advice.
This enables you to avoid and manage issues, quickly relieving your inhibiting lifestyle conditions when complications arise. We personalize patient care plans based on each patient’s condition and unique circumstances. Wellness and Pain can help improve wellness, increase mobility, relieve pain, and enhance your mental space and overall health.