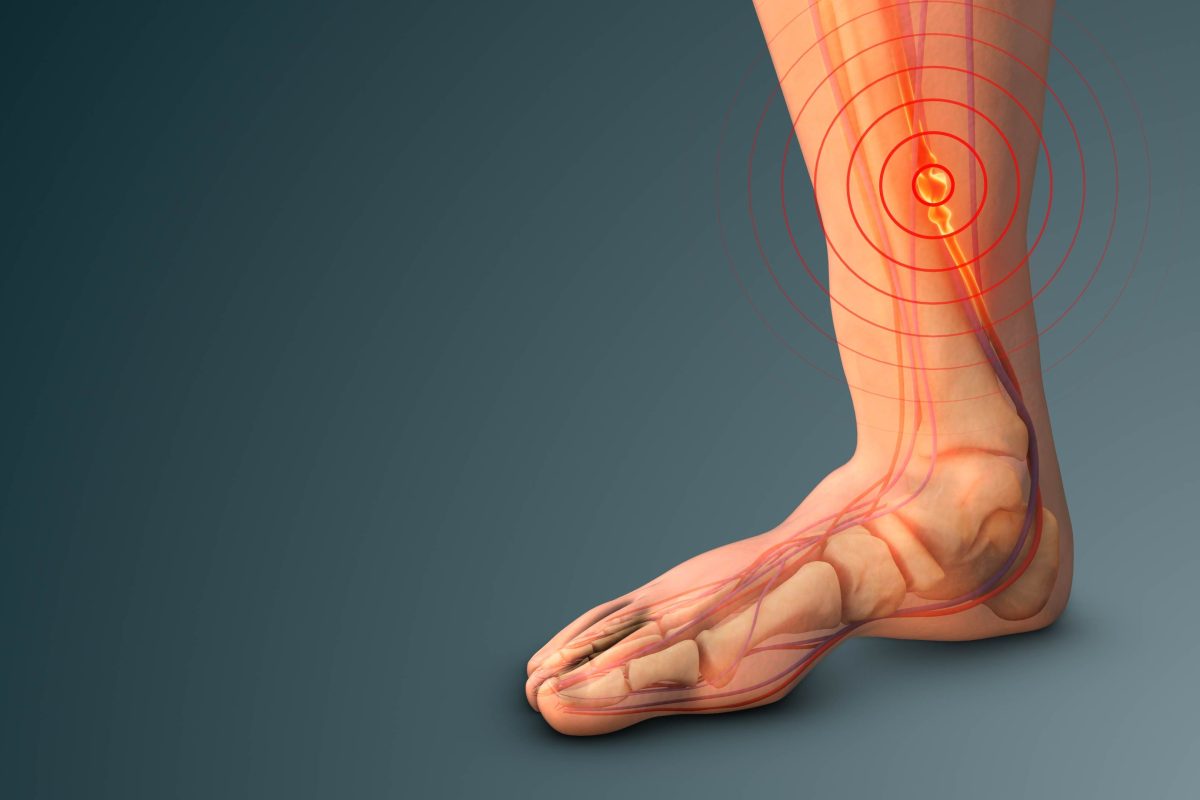
Sciatica and lower leg pain begins in the lower back and travels down one leg, accompanied by tingling, numbness, or bursts of discomfort. These sensations occur when the sciatic nerve becomes irritated or compressed along its path.
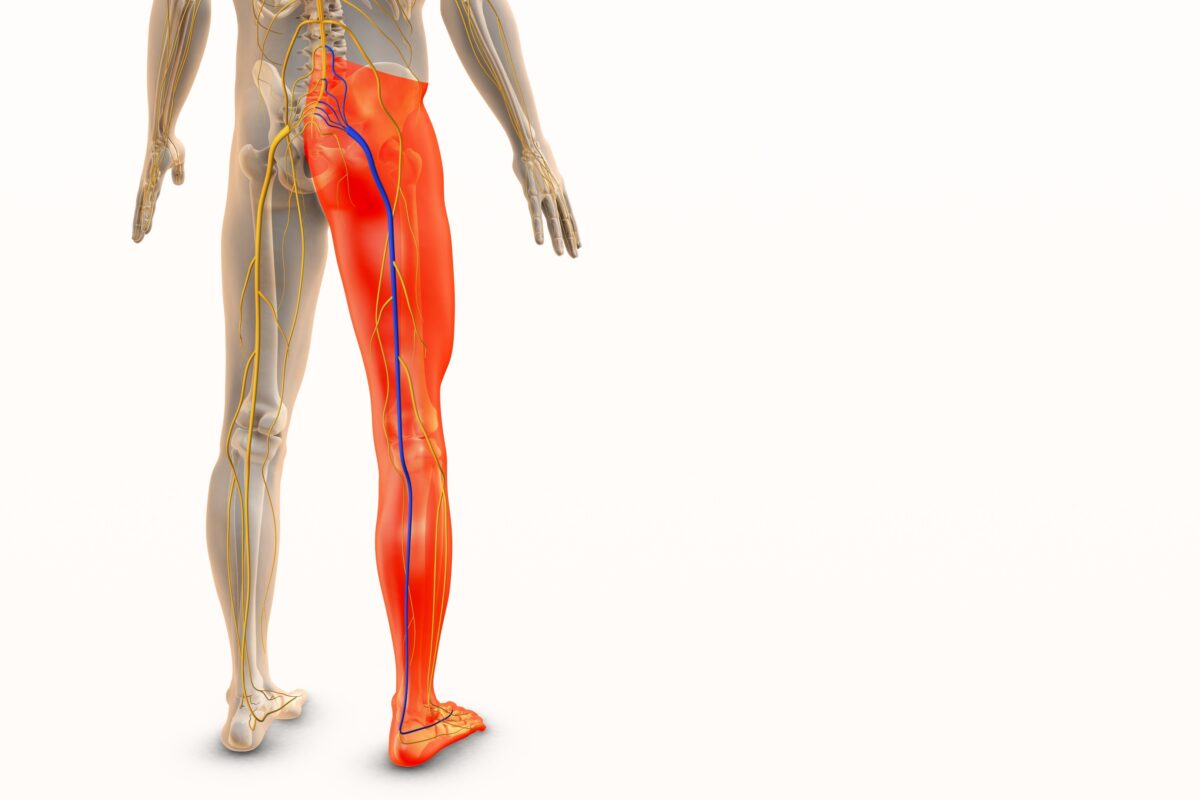
This nerve, the largest in the body, runs from the lower spine through the hips and gluteal muscles, continuing down to the foot. Nearly half of people worldwide will experience sciatica at some point.
While many associate it with aging, it’s increasingly common among younger adults as well. Hours spent sitting at a desk, leaning over a laptop, or maintaining poor posture can all contribute. The way we move, or fail to move, sets the stage for how this nerve behaves.
“Furthermore, as the global population ages, the number of people suffering from sciatica and lower back pain is increasing, which is driving demand for treatment options and propelling the growth of sciatica treatment market,” according to Yahoo Finance. “Also, increasing disposable incomes and better access to healthcare, allows people to seek medical treatment for sciatica symptoms. In addition, increasing awareness of sciatica and its symptoms, as well as the availability of better diagnostic and treatment options, is also driving growth in the sciatica treatment market.”
Sciatica and Lower Leg Pain: The Spectrum of Symptoms
If you’re dealing with sciatica and lower leg pain, know that the sciatic nerve plays a huge role in movement and sensation. Originating from several spinal levels, known as L4 through S3, its thick bundle travels through the pelvis and into the legs.
Because it stretches so far, a problem in one part of its course can send shockwaves to another. What feels like pain in the calf or foot can actually come from a compressed nerve root higher up in the lower back. This is what makes sciatica so tricky — it often hurts far from where it begins.
No two experiences of sciatica feel exactly alike. For some, the pain is sharp or burning, tracing a path down one leg. Others describe a strange tingling sensation, almost like static dancing across the skin.
The location of discomfort depends on which portion of the sciatic nerve is compressed. In many cases, pain radiates along the back of the thigh.
For others, it stretches into the calf, ankle, or even the toes. Each person’s pattern tells a slightly different story about where the nerve is being affected.
- L4 Compression: Pain may radiate to the hip and the front of the thigh.
- L5 Compression: Discomfort often travels to the big toe and the top of the foot.
- S1 Compression: The sensation typically reaches the outer side of the foot and the pinky toe.
In more severe cases, muscle weakness can develop. Some people notice difficulty lifting the front of the foot or standing on their tiptoes, which are clear signs that the nerve’s signals are being disrupted.
Prompt medical evaluation at that stage is important to prevent long-term problems.
Comparing Common Sciatic Triggers
Many patients suffering from sciatica and lower leg pain describe sciatica in similar terms, but the real story lies in what’s happening beneath the surface.
Pain is a signal, not the root problem. A herniated or slipped disc may press on a nerve root, while bone changes in the spine or joint degeneration can create similar pressure.
In some cases, tight or inflamed muscles near the lower back or pelvis compress the nerve as it travels outward. Each cause requires its own approach to achieve lasting relief.
The chart below outlines common causes and how treatment options can differ. Still, only a physical evaluation — and sometimes imaging — can provide the full picture needed for the best path to recovery.
| Primary Mechanism | Characteristic Sensation | Typical Aggravating Factor | |
| Herniated Disc | Inner disc material leaks and presses on the nerve root. | Sudden, electric-like shooting pain. | Bending forward, coughing, or sneezing. |
| Spinal Stenosis | Gradual narrowing of the bony canal where nerves reside. | Cramping, heaviness, or claudication in both legs. | Prolonged walking or standing perfectly upright. |
| Piriformis Syndrome | A small muscle in the buttock tightens or spasms over the nerve. | Deep, localized ache in the hip/glute that radiates down. | Sitting on hard surfaces or driving for long periods. |
| Spondylolisthesis | One vertebra slips forward over the one below it. | Persistent ache with occasional sharp, mechanical jolts. | Arching the back or heavy lifting. |
| Degenerative Disc Disease | Wear and tear causes discs to lose height and stability. | Chronic, low-level grumbling pain with periodic “flare-ups.” | Long periods of inactivity or static posture. |
Understanding which factor is at play helps shape the right treatment plan. Simply treating the pain lower down often misses the real source.
Identifying your particular symptom pattern allows your pain management specialist or doctor to target the underlying issue effectively.
Biological Mechanics of Sciatica and Lower Leg Pain
That sharp, burning sciatica and lower leg pain is your nervous system’s way of signaling that something is wrong. When a nerve is squeezed or irritated, it sends distress signals along its entire length.
If this goes on for too long, the brain can start to overreact to those signals. This is a process called central sensitization, where the nervous system effectively turns up the volume on pain.
The sciatic nerve also depends on a steady supply of oxygen-rich blood to function well. When blood flow is restricted, the nerve becomes stressed quickly, much like the tingling you feel when a foot falls asleep, only more intense and harder to ignore. Prolonged pressure can damage the nerve’s protective myelin coating, which normally helps signals travel smoothly.
As that coating frays, signals begin to misfire or leak, and people often notice sudden, shooting, or electric pains. In more advanced cases, the inner fibers of the nerve can be injured, leading to persistent numbness or loss of sensation.
Irritated nerves may also release chemicals that trigger local inflammation, making the surrounding area tender so that even light touch feels exaggerated or uncomfortable.
“In the gluteal region, the sciatic nerve is supplied by the inferior gluteal artery and cruciate anastomosis (the medial and lateral circumflex femoral arteries, inferior gluteal artery and the first perforating branch of the profunda femoris artery),” states Physiopedia. “Lower in the thigh, arterial branches derived from the perforating branches of the profunda femoris artery or the anastomotic chain between them or, occasionally, from the popliteal artery, enter the nerve on its lateral or anterolateral side.”
To stay healthy, the sciatic nerve relies on tiny blood vessels called the vasa nervorum, which carry oxygen and nutrients directly to the nerve tissue. When these vessels are damaged or blocked, the nerve cannot perform properly. Conditions such as diabetes can injure these small vessels over time, contributing to numbness, tingling, and other nerve symptoms that can mimic or worsen sciatica.
Anatomy adds another layer of complexity. Not everyone’s sciatic nerve follows the same path. A notable minority of people have natural variations in how and where the nerve forms and divides as it passes near the hip muscles. In some, the nerve splits earlier than usual; in others, part of it passes through or around the piriformis and nearby muscles.
These differences are not harmful on their own, but they may slightly increase the risk of the nerve being compressed, especially in people who frequently lift heavy objects or repeat certain athletic movements.
Finding the Root Cause of Your Issues
Spotting sciatica and lower leg pain, especially the underlying health problem, involves more than simply describing where it hurts. Doctors use specific stress tests to understand what the nerve is doing and where it might be irritated.
One of the most common is the Straight Leg Raise (SLR). During this test, you lie on your back while your clinician slowly lifts your straight leg. If your familiar shooting pain appears between about 30 and 70 degrees, it often suggests that a lumbar disc is pressing on a nerve root.
A hands-on exam is always the starting point, but imaging can add important detail. MRI or CT scans can show discs, nerves, and other soft tissues that a standard X-ray cannot. At the same time, scans often reveal findings that many people have without any pain at all, so results must be interpreted carefully.
Most clinicians focus on your symptoms and function first, then use imaging to support what they already suspect. If the exact source of nerve irritation is still unclear, nerve tests such as EMG and nerve conduction studies can help map how well signals travel through your muscles and nerves, and where they may be getting blocked.
Dealing with sciatica doesn’t mean you have to give up travel or favorite activities. With some planning, you can usually stay active and comfortable.
Long stretches of sitting or slouching in the same position can tilt the pelvis and increase pressure on the nerve, so building in brief movement breaks is important. Standing up every 30 minutes, even for a minute or two of gentle walking or back stretches, can ease strain on your spine.
“Some experts suggest that prolonged sitting is more dangerous than smoking,” states Physioinq. “And while this sounds extreme, sitting for long periods can do damage to our health in ways we might not realize. As modern lifestyles become more and more sedentary, sitting for long periods of time can cause major issues to your spine. Somewhere between one and ten per cent of the population ages 25 to 45 report sciatica pain, one of the most painful risks of prolonged sitting.”
Simple tools can make a real difference when you are on the go. Gentle stretching keeps you moving more freely, and many people find it helpful to pack a stretch strap or thin yoga mat for hotel rooms or layovers. On flights, small adjustments like using a footrest or foot hammock to elevate the legs and a lumbar travel pillow or seat cushion to support the lower back can reduce stress on the sciatic nerve.
Day-to-day support also helps prevent flare-ups. If you spend hours on your feet, a well-fitted hip or sacroiliac brace can improve alignment and reduce strain. A firm massage ball can release tight muscles in the buttock area that sometimes press on the nerve, and warm packs or topical pain-relief creams may ease local discomfort.
These measures do not replace medical care, but they can offer quick relief and help you stay more comfortable between visits.
Sciatica and Lower Leg Pain: Frequently Asked Questions
- How long does a typical sciatica flare-up last? Most acute episodes resolve within four to six weeks with conservative care. However, if the underlying cause is a chronic structural issue like stenosis, symptoms may fluctuate over a longer period, requiring ongoing management strategies.
- Is bed rest the best way to recover? Actually, modern medical consensus suggests that prolonged bed rest can be counterproductive. While a day or two of reduced activity might be necessary during extreme pain, gentle movement and walking are generally encouraged to keep the muscles from stiffening and to promote healthy circulation to the nerve.
- When should I consider my leg pain a medical emergency? You should seek immediate medical attention if you experience red flag symptoms, such as sudden loss of bladder or bowel control, significant weakness that makes walking impossible, or numbness in the saddle area (inner thighs and groin).
- Does a diagnosis of sciatica always lead to surgery? Not at all. The vast majority of patients, or 80-90 percent, find significant relief through non-surgical means, including physical therapy, anti-inflammatory medications, and epidural steroid injections. Surgery is typically reserved for cases where neurological deficits are progressing or pain is completely unresponsive to conservative measures.
Living with sciatica often means balancing different treatments and strategies over time. One person might feel fine during routine days, yet notice their pain flare quickly on a long flight. Trapped in a narrow seat with little room to shift or stand, the nerve irritation can build fast.
Planning ahead can make a long trip far more manageable and comfortable.
Wellness and Pain
Get rid of your sciatica and lower leg pain by visiting Wellness and Pain. We offer conservative treatments, routine visits, and minimally invasive quick-recovery procedures. We can keep you free of problems by providing lifestyle education and home care advice.
This enables you to avoid and manage issues, quickly relieving your inhibiting lifestyle conditions when complications arise. We personalize patient care plans based on each patient’s condition and unique circumstances. Wellness and Pain can help improve wellness, increase mobility, relieve pain, and enhance your mental space and overall health.