Some pain fades with time, but some lingers. It comes when you wake up, try to sit still, reach for a grocery bag, or climb the stairs. After a while, it starts shaping your days in quiet, frustrating ways.
Maybe you’ve tried physical therapy, over-the-counter meds, or rest. Maybe nothing’s worked for very long. If that sounds familiar, you might be wondering what your next option is.
That’s where pain management physicians step in. They focus on identifying the source of your pain and creating treatment plans that help you function again.
In this guide, you’ll learn what they do, when to see one, and how the right care can make daily life manageable.
What Is a Pain Management Physician?
A pain management physician is a medical doctor who specializes in evaluating and treating pain that lasts longer than expected or doesn’t improve with basic care. Their focus is not just on easing discomfort but on understanding where the pain is coming from and how it’s affecting your daily life.
These doctors often treat people who have already seen other specialists or tried treatments like rest and physical therapy without much progress. In many cases, the pain is linked to nerves, joints, or musculoskeletal problems that aren’t always obvious during routine exams.
What makes pain management physicians different is their training and approach. They use detailed physical examinations, imaging studies, and patient history to guide their decisions. Then they prescribe treatment based on what’s happening in the body.
Whether your pain started after an accident or slowly built over time, these specialists work to identify the source and provide lasting relief. They offer a wide range of options, from conservative care to targeted procedures, to help you move, rest, and function more comfortably.
Common Conditions Treated by Pain Management Doctors
Pain management doctors are trained to figure out the source and match it with the right type of care. They see various conditions, from everyday issues to more difficult or uncommon diagnoses.
Some of the most common conditions they treat include:
- Chronic pain that lasts beyond the normal healing time, often without a clear cause
- Back and neck pain, which may be related to disc issues, posture, or strain
- Joint pain from arthritis, inflammation, or overuse
- Nerve pain, including sciatica and conditions like complex regional pain syndrome
- Post-surgical pain that continues long after recovery
- Headaches or migraines that are linked to nerve irritation or muscle tension
- Musculoskeletal pain, which includes pain in the muscles, ligaments, tendons, and bones
Pain doesn’t always show up on imaging. That’s why pain management specialists look beyond scans and test results to understand how pain affects your movement, sleep, and daily function.
If you’ve been living with any of these symptoms and haven’t found consistent relief, it might be time to explore more targeted care.
Treatment Options in Pain Management
Pain affects everyone differently. What helps one person may not help another, which is why pain management doctors offer a wide range of treatments. The goal is to match the care to the source of the pain, the way it affects your life, and how your body responds.
Depending on your condition, your treatment plan may include:
Conservative and Non-Invasive Therapies
- Physical therapy to build strength, improve mobility, and ease tension in painful areas
- Muscle relaxants or anti-inflammatory medications to support short-term recovery
- Education around body mechanics, pacing, and managing flare-ups throughout the day
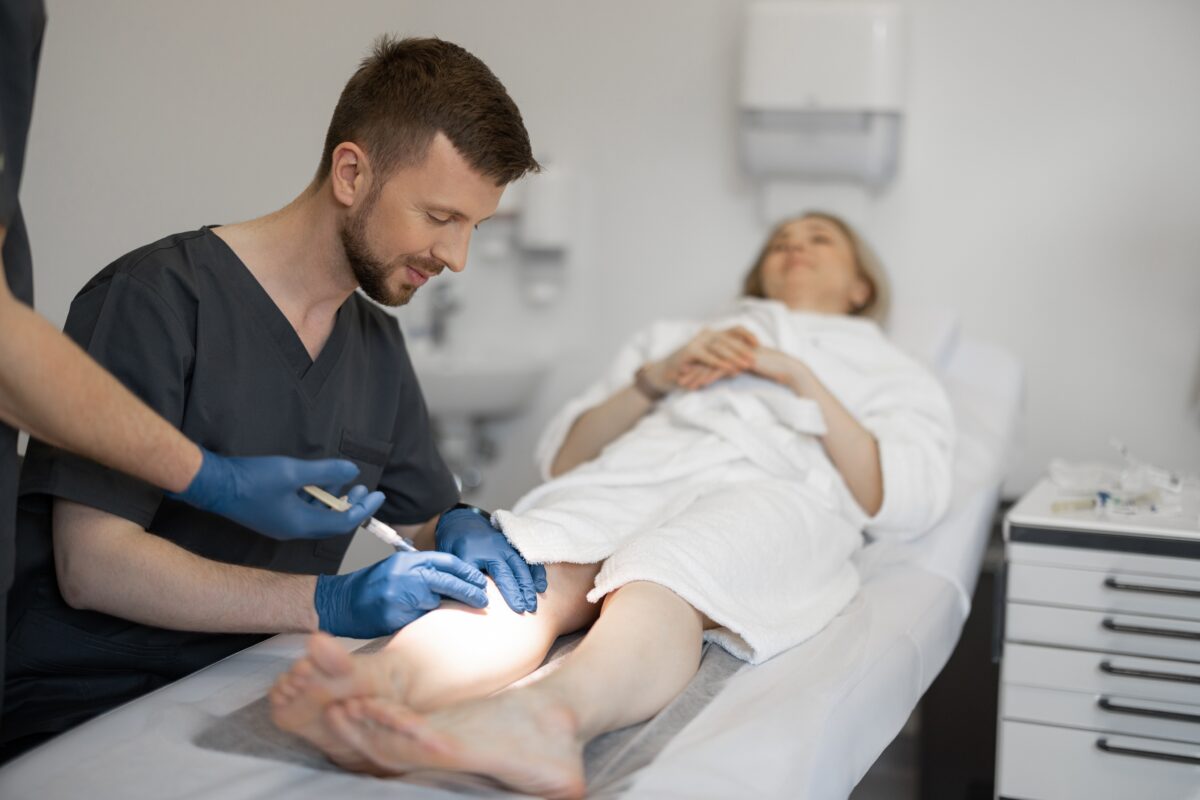
Injection-Based Treatments
- Nerve blocks that deliver medication directly to the area where pain signals begin
- Joint injections to reduce swelling and discomfort in joints like the knees, hips, or shoulders
- Epidural steroid injections for nerve-related back or leg pain
Interventional Procedures
- Radiofrequency ablation to quiet overactive nerves that keep sending pain signals
- Spinal cord stimulation and dorsal root ganglion stimulation for severe or difficult-to-treat nerve pain
- Peripheral nerve stimulation for pain that’s limited to one area and hasn’t improved with other treatments
Medication Management
- Selective use of opioid medications, when appropriate, under close supervision
- Additional options like antidepressants, nerve pain medications, or sleep support, depending on your symptoms
Pain management doctors often combine several of these options over time. They also collaborate with physical therapists and other providers to help you regain strength and function safely.
What to Expect From Your First Visit
Your first visit to a pain management doctor is about getting the full picture. You’ll talk through when the pain started, how it feels, what makes it worse or better, and how it affects your daily routine. The doctor will review your medical history, including any treatments or medications you’ve tried in the past.
A physical examination will help assess your movement, strength, nerve responses, and areas of tenderness. If needed, the doctor may order imaging tests or nerve studies to look more closely at what’s happening inside the body.
You won’t be rushed into a procedure. Instead, the goal is to gather the right information, explain what’s going on, and work with you to plan the next steps.
How to Find the Right Pain Management Doctor
Ask your primary care provider for a referral. You can also check with your insurance provider to find specialists in your network. Look for doctors who are board-certified in pain medicine, and don’t hesitate to ask about their experience with your specific condition.
Reading patient reviews can give you insight into a doctor’s communication style, availability, and overall care philosophy. Many of the top pain management doctors are part of multidisciplinary clinics that offer a range of services in one place.
It also helps to prepare questions ahead of your visit. You might ask what treatments they typically use, whether they collaborate with physical therapists or other specialists, and how they measure progress over time.
Common Misconceptions About Pain Management Doctors
Many people hesitate to see a pain specialist because of common misunderstandings. These misconceptions can prevent patients from getting the help they need.
Myth 1: Pain doctors only prescribe opioid medications.
One of the most frequent myths is that pain doctors only prescribe opioid medications. While these may be part of a treatment plan in some cases, they’re not the default. Pain specialists use a wide range of tools, many of which are non-medication-based, to help reduce pain and restore function.
Myth 2: Pain doctors are a last resort.
Another misconception is that pain doctors are a last resort. In reality, they can be most effective when involved early, especially for complex or worsening symptoms.
Myth 3: Pain specialists only treat severe conditions.
Some also believe that pain specialists only treat severe conditions. But they regularly work with people who have moderate pain that interferes with everyday life, from muscle strain to post-surgical discomfort.
If you’ve delayed seeing a specialist because of these beliefs, it may be worth taking a second look. The goal of pain medicine is to treat the whole person, not just hand out prescriptions.
Get Help From a Full Team of Specialists at Wellness and Pain
If you’ve been living with pain that keeps coming back or never fully goes away, it’s time to visit a pain management physician.
At Wellness and Pain, you’ll find a full team of board-certified physicians, pain specialists, neurologists, chiropractors, and wellness providers who work together to find what’s causing your pain and how to treat it.
We offer conservative care like chiropractic, massage, and acupuncture, along with advanced options such as nerve blocks, joint injections, spinal procedures, and regenerative therapies like platelet-rich plasma (PRP) and stem cells. Every plan is personalized, based on your symptoms, health history, and response to care.
You’ll also have access to thorough diagnostics, including electromyography (EMG) nerve studies, high-resolution imaging, and targeted injections to identify pain that doesn’t show up on routine scans.
Struggling with pain? Wellness and Pain can help you understand the cause, treat it effectively, and start feeling better.
FAQs About Pain Management Physicians
What is a pain management physician?
A pain management physician is a medical doctor who specializes in diagnosing and treating pain caused by injuries, illnesses, or underlying conditions. They use a range of techniques to provide long-term pain relief without relying solely on medication.
What not to say to a pain management doctor?
Avoid vague phrases like “everything hurts.” Instead, be specific about where you’re experiencing pain, what makes it better or worse, and how it affects your life. Clear details help your doctor decide how to address your symptoms more effectively.
What type of doctor is best for pain?
It depends on the source of the pain. For joint and movement issues, an orthopedic specialist may help with orthopedic pain. For broader or nerve-related pain, a board-certified pain management physician who offers interventional treatments is often the most comprehensive option.
What are the three types of pain management?
Pain is typically managed through medication, physical or behavioral therapy, and interventional treatments such as nerve blocks or spinal procedures. These are especially helpful for both acute pain and more persistent issues.
Where can I find experienced pain management physicians in Pennsylvania?
Patients searching for expert care often turn to the pain management physicians’ Harrisburg office or the pain management physicians’ Philadelphia office for specialized treatment. Both locations are part of Pennsylvania’s top pain management providers, offering care grounded in the latest research and tailored to individual needs.
Services at these offices may include advanced procedures (such as epidural steroid injections) Pennsylvania patients frequently rely on for nerve-related or spinal pain.
What if my pain doesn’t improve after a short period of treatment?
If your symptoms continue beyond a short period, it’s important to follow up with your doctor. Sometimes pain is linked to deeper issues that require more advanced evaluation.
Clinics that are consistently ranked for patient outcomes often use diagnostic tools and therapies that help avoid unnecessary surgery, making sure your care stays focused on safety and long-term recovery.